
If you’re a man over 50 reading this with a cup of coffee in one hand, there’s a fair chance you’ve already been up to the bathroom once or twice this morning. Maybe last night, too. Three times, perhaps. And the stream isn’t quite what it used to be — that confident arc of your thirties has turned into something more like a garden hose someone forgot to turn fully on.
Welcome to the club. It’s a big one. Most men over 60 are already members, and most of them haven’t told anyone.
What we’re talking about here is BPH — benign prostatic hyperplasia, which is a fancy way of saying “your prostate has been quietly growing for years and is now squeezing your urinary plumbing.” It’s not cancer. It’s not dangerous in itself. But it can absolutely ruin your sleep, your golf game, and your willingness to sit through a long film at the cinema.
I see expats in Pattaya every week who’ve been putting up with this for years. Some of them genuinely thought it was just “part of getting older” and that nothing could be done. Others tried the pills, didn’t like the side effects, and quietly gave up. A few even started planning their lives around the nearest toilet — which is no way to enjoy retirement on the Eastern Seaboard.
So let me tell you about an option that, in my opinion, doesn’t get talked about enough out here: HoLEP.
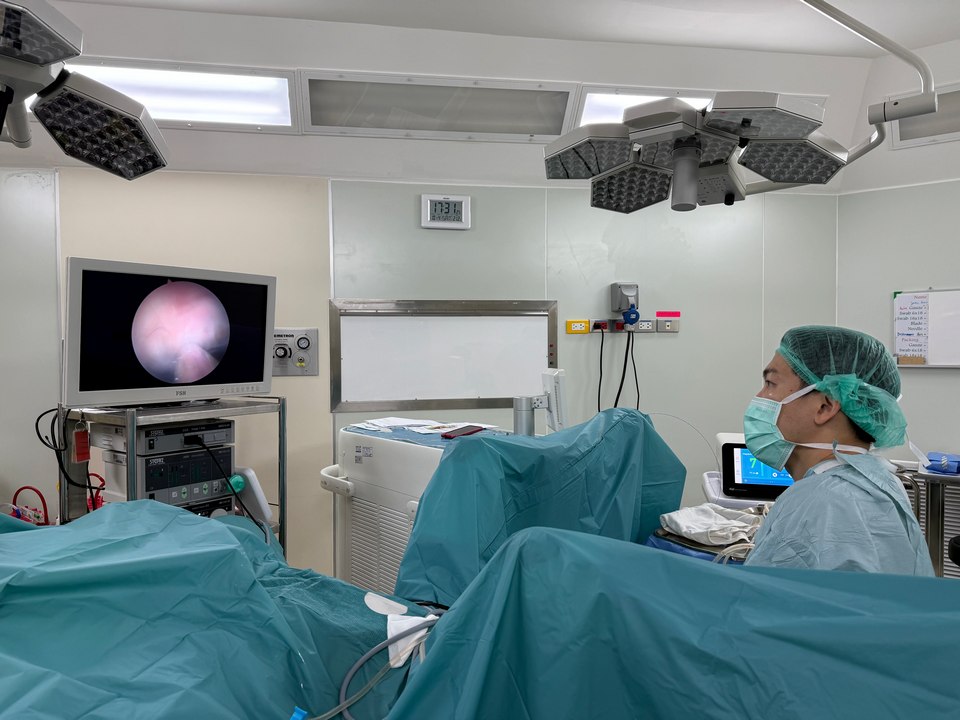
HOLEP — A LASER, NOT A SCALPEL
HoLEP stands for Holmium Laser Enucleation of the Prostate. The name is a mouthful, but the procedure itself is surprisingly elegant. It was developed in New Zealand in the late 1990s, and it has quietly become one of the best-studied prostate operations in the world.
Here’s the simple version of what happens: you go to sleep under general anaesthetic. We pass a small telescope through the urethra — no cuts, no stitches on the outside. A holmium laser then peels out the obstructing core of the prostate in one piece, almost like coring an apple. The tissue is removed, the prostate channel is wide open again, and most patients are home within a day or two.
What I like about HoLEP, and what I tell my patients, is that it’s a one-and-done procedure for most men. The chance of needing it redone is less than 1% over ten years. Compare that to TURP — the older operation many men are familiar with — where 10 to 15% of patients need a second go-round. That’s a real difference when you’re 65 and would rather not be back in hospital at 75.
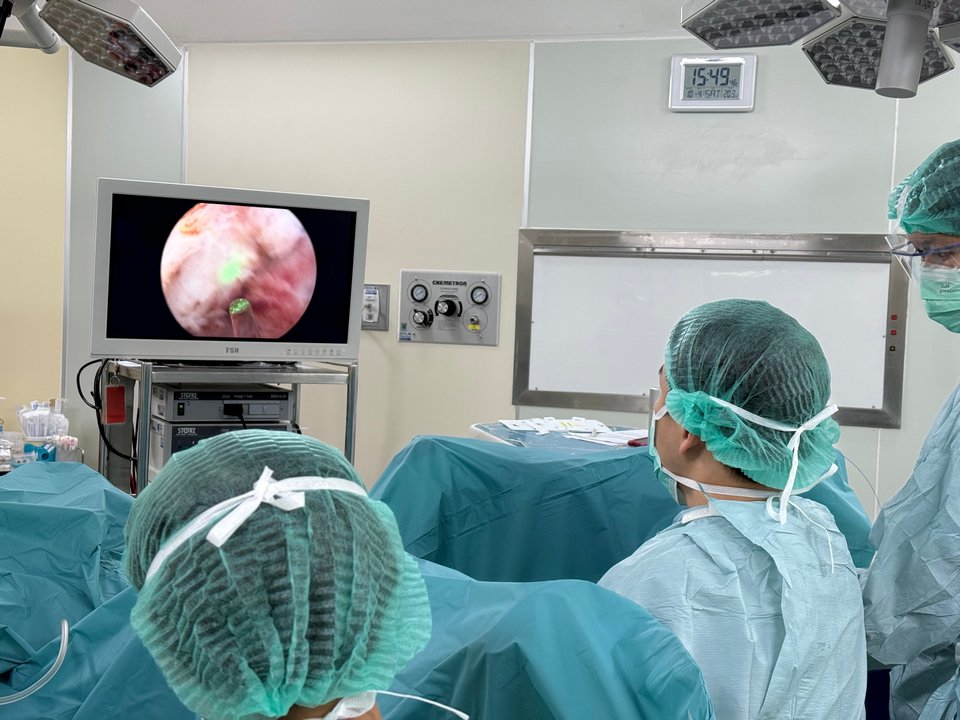
WHO IS THIS FOR?
Honestly? Most men with significant BPH symptoms. Weak stream. Stop-and-start urination. The feeling that you haven’t quite finished. Getting up at night more than once or twice. Straining. The sense that life now revolves around the location of the nearest gents.
It’s also a good option for men whose prostates have got too big for other treatments — and frankly, after a few decades of growth, many of them have. Unlike most other endoscopic options, HoLEP works regardless of prostate size. Small, medium, large, or “good grief” — it doesn’t matter.
It’s also a strong choice for men who’ve tried medications and either got tired of taking them every day, didn’t get enough relief, or didn’t like the side effects. Some of those drugs can affect blood pressure, libido, or ejaculation, and not every man wants to trade one problem for another.
WHAT TO EXPECT
I’ll be honest with my patients about the recovery, because nobody likes surprises after surgery. You’ll wake up with a catheter — that thin tube draining the bladder — which usually comes out the next day. About 90% of men go home without it. Some can even leave the same day, though I generally prefer one night in hospital just to be safe.
For the first week or two, you’ll see some blood in the urine, on and off. This is normal. There may be some burning when you urinate. This too is normal. It’s not an infection, and it settles. The frequent and urgent need to urinate — which has often been with you for years — usually takes about three months to fully calm down. The bladder has been irritable for a long time, and it needs a bit of time to relearn what “normal” feels like.
One thing I always discuss before surgery: about 90% of men experience what we call retrograde ejaculation afterwards. The plumbing still works, the orgasm is the same, but the fluid travels backwards into the bladder rather than out. It’s harmless and it comes out with the next urination. For most men of the age we’re talking about, this isn’t a deal-breaker. But it’s a real change, and it’s only fair to know about it before, not after.
Erectile function is not affected by HoLEP. Whatever you had going in, you’ll have going out. That’s worth saying clearly because there’s a lot of confusion about prostate surgery and erections — that confusion mostly comes from cancer surgery, which is a completely different operation.
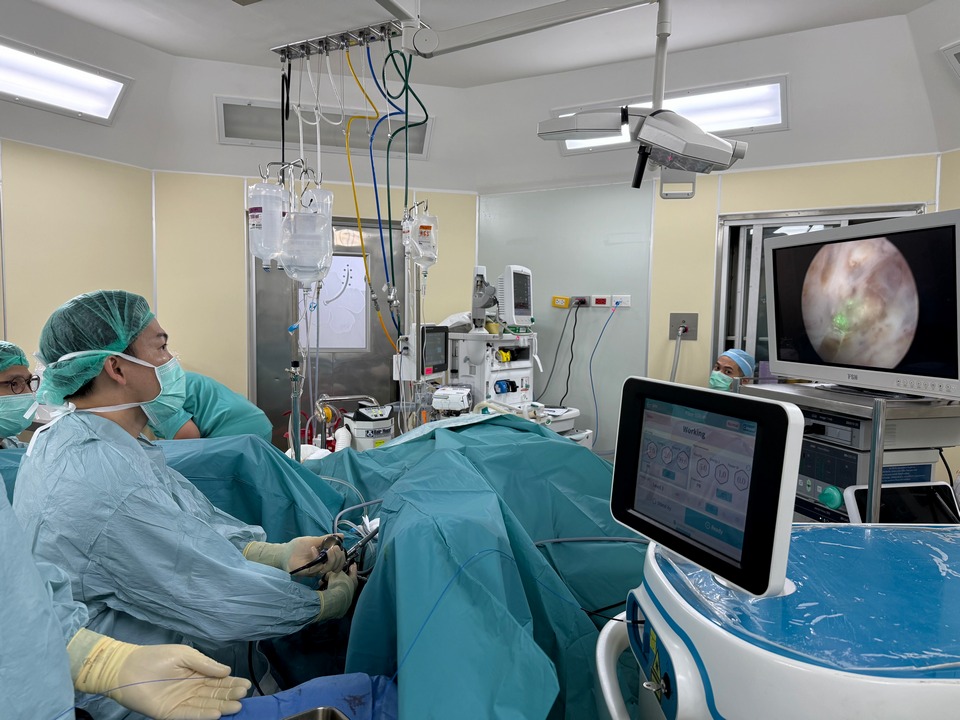
WHY I’M WRITING THIS
Because too many men in this town have been quietly putting up with something that doesn’t need to be put up with. I’ve had patients in their 70s tell me, after surgery, that they hadn’t slept through the night in a decade. One gentleman from the UK said he’d forgotten what it felt like to leave the house without a mental map of every public toilet between his condo and the beach.
Pattaya has come a long way in the last 20 years when it comes to specialist medical care. The technology used in good urology centres here is the same technology you’d find in London, Sydney, or Berlin.
If you’ve been getting up three times a night, or hovering at the urinal hoping things will start moving, do yourself a favour. See a urologist. It doesn’t have to be me — just see someone. A simple flow test and an ultrasound will tell you most of what we need to know. From there, you have options. Tablets, lasers, or just keeping an eye on things. None of it is scary. None of it is rushed.
But please stop assuming this is just how it has to be. It isn’t. And life on this side of 60 is too good to spend half of it looking for a bathroom.
Dr. Niti Navanimitkul is a consultant urologist based in Pattaya. He performs HoLEP at the Bangkok Hospital Pattaya. And other Minimally invasive surgery for BPH such as Rezum, UroLift at his private clinic in Pattaya.
Booking for consultation at my private clinic at email: [email protected]
If you are experiencing ED, direct private email to Dr. Niti Navanimitkul, a Sexual Dysfunction Specialist and Penile Prosthesis Surgeon from Men’s Health Thailand (Pattaya)


















