The author of this articles notes that “my father-in-law was just relaxing after his dinner when he slid from his chair and was dead within the hour. No warning. Yes, he was a smoker, male in his late 80s, so perhaps it was not surprising that the cause was Abdominal Aortic Aneurysm. At least it wouldn’t have been a surprise to those who heard Dr. Sujit Banyatpiyaphod, Cardio Vascular Surgeon and Director of the Heart Centre, Bangkok Hospital Pattaya in his talk to the Pattaya City Expat Club at their Sunday, June 2, meeting. Dr. Sujit set the tone by saying artery disorders, if left unchecked, can lead to disability or death.
Abdominal Aortic Aneurysm is something that is more likely to occur as one gets older, especially if one is male, smokes, has a history of high blood pressure, and diabetes. It is less common in women as they are protected by the hormone estrogen before menopause. However, if it does occur in a woman, it is more likely 10 years later, and more likely to be fatal. As there is no advance warning, it is urgent to get to the hospital as quickly as possible if suffering an intense, sharp, stabbing pain in the abdomen, flank or back. If rupture occurs before reaching the hospital, it is usually fatal. Surgery will be undertaken immediately.
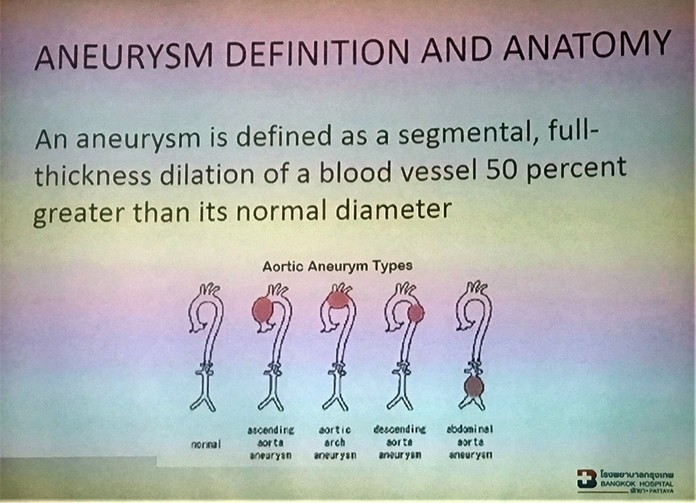
Early detection and diagnosis are increasingly available and now, aortic aneurysms can best be detected by lower abdominal ultrasound screening. The Heart Centre BHP kindly offered a complimentary screening for 60 members who are at risk of having abdominal aortic aneurysms. Aortic Aneurysms are life threatening and usually asymptomatic; aneurysms that produce symptoms are at an increased risk for rupture which is associated with a higher mortality rate; risk of a rupture increases with the number of risk factors: smoker, male, advancing age, family history of aortic problems, atherosclerosis and if the initial aneurysm is large (>5.5cm.) in diameter; if treated before it ruptures, the success rate of treatment is over 95%. If an aneurysm is detected in an ultrasound and it is not large, it should be checked regularly to detect any expansion.
Dr. Sujit emphasized the importance of having annual medical checkups. He suggested as an extra, including a lower abdominal ultrasound which would detect an aneurysm as well as problems such as kidney stones or gall stones. Aneurysms may occur in any blood vessel but the abdominal aorta is most frequent. The aorta is the main artery of the body, directly connected to the heart and taking the majority of the blood from the central pump to the abdominal organs and the legs. This artery is around 2 cms in diameter. Occasionally, the artery begins to bulge and can grow to 4 or 5 times the normal diameter. This is known as an aneurysm and may show as a thickness dilation, and sometimes as a balloon on the artery. This can burst causing a catastrophic internal hemorrhage. Aneurysms are caused by a weakening or damage in the wall of a blood vessel. An aneurysm may be discovered as a result of screening in high risk population or an incidental finding during radiology or surgery.
There are 2 approaches for repair. The traditional surgical approach involves a large incision in the abdomen where aortic aneurysm is identified and cut out. The traditional Open Repair involves a large incision in the abdomen to directly visualize the abdominal aorta and replace and repair the aneurysm. The missing piece of the aorta is replaced with a synthetic graft. The open repair is considered the surgical standard for an abdominal aorta aneurysm repair. A tube graft may be used to repair the aneurysm. Grafts are from Dacron or PTFE (synthetic). CAT Scans are used to check the tightness of the endovascular graft. They are also useful to doctors in planning aneurysm repair surgery.
The second approach is placing an endovascular graft in the artery. A catheter or tube is threaded into the femoral artery in the groin and the graft is positioned so that it spans and sits inside the aneurysm and protects it from expanding. It reduces recovery time but it is costly. Dr. Sujit also said it can’t be used for all types of aneurysms. The location or size of the aneurysm may prevent a stent or graft from being safely or reliably placed inside the aneurysm.

The treatment plan depends on the individual. Dr. Sujit stressed the importance of life long control of risk factors: smoking, diabetes, hypertension, high cholesterol, body mass index over 27. He concluded his very informative talk by answering questions from the audience. PCEC Chairman Roy thanked Dr. Suijit and on behalf of the Club presented him with a Certificate of Appreciation.
This was followed by announcements and news of special interest groups, then the Open Forum where the audience can ask questions or make comments about expat living in Thailand, especially Pattaya.

 |
 |
 |